Video Doctor Visit — What to Expect on Your Online Appointment
A video doctor visit lets you see a licensed Canadian physician face-to-face through a secure video call — without travelling, sitting in a waiting room, or risking exposure to other illnesses. If you have never had one before, you may wonder how the call actually works, what doctors can see through a camera, what they cannot, and what equipment you need. This page walks you through the entire experience step by step: setting up your device, joining the call, what your doctor can assess visually, how privacy is protected, and how to prepare so your appointment runs smoothly the first time.
Book Your Appointment Now
A video doctor visit is a secure, encrypted video appointment with a licensed Canadian physician. You join from a phone, tablet, or laptop with a camera, microphone, and basic internet. The doctor takes a history, performs a focused visual exam, and creates a treatment plan. Most visits run 10-20 minutes and cover prescriptions, sick notes, lab requisitions, and referrals.
- Most video visits last 10-20 minutes from join to wrap-up
- Works on any modern smartphone, tablet, or laptop with a camera and 1.5 Mbps internet
- Consultations may be covered by AHCIP for eligible Alberta residents
- Encrypted platform meeting PIPEDA and provincial health privacy standards
What Is a Video Doctor Visit?
A video doctor visit is a real medical appointment conducted over a secure, encrypted video call instead of in person. You and a licensed Canadian physician see and hear each other in real time through your phone, tablet, or laptop camera. The visit follows the same clinical structure as a clinic visit — your doctor takes a history, performs a visual assessment, makes a diagnosis where appropriate, and creates a treatment plan.
Video visits are the standard format for virtual care in Canada because seeing a patient adds clinical information that a phone call cannot. Your doctor can observe your skin, your eyes, the way you breathe, swelling, posture, and how you appear overall. For most non-emergency concerns, this is enough information to diagnose and treat safely.

What a Video Doctor Visit Actually Looks Like
Here is what happens from the moment your appointment time arrives.
A few minutes before your scheduled time, you receive a secure link by email or text. Tap the link from the device you want to use. The browser or app asks permission to use your camera and microphone — say yes, otherwise the doctor will not be able to see or hear you. You enter a virtual waiting room until your physician joins.
When the doctor connects, you see their face on screen and they see yours. The visit opens like any clinic appointment: confirmation of your identity and health card, a question about what brought you in today, and a focused conversation about your symptoms. If something needs to be looked at — a rash, an eye, a sore throat, swelling — your doctor will ask you to move closer to the camera, adjust the lighting, or angle your phone. Most visits last 10 to 20 minutes. At the end, prescriptions are sent to your pharmacy and any documents (sick notes, requisitions, referrals) are emailed to you.

Technology Requirements — What You Need for the Call
You do not need anything fancy. Most patients use the phone already in their pocket. Here is what works well.
- A device with a camera and microphone — smartphone, tablet, or laptop. Smartphones are the most common choice because they are easy to move around to show your doctor a specific area.
- A reasonably modern web browser — Chrome, Safari, Firefox, or Edge updated within the last year or two. No special app download is required for most visits.
- An internet connection of at least 1.5 Mbps upload and download — most home Wi-Fi and modern mobile data (LTE or 5G) is more than enough. You can test your speed at fast.com in 30 seconds.
- A quiet, private space where you can speak openly — bedroom, parked car, home office, or any room with a closing door.
- Good lighting — face a window or lamp rather than having a bright light behind you, which puts your face in shadow.
- Headphones or earbuds (optional but helpful) — they improve audio clarity and add privacy if others are nearby.

What Your Doctor Can — and Cannot — See on Video
Understanding the limits of video helps you use the appointment well.
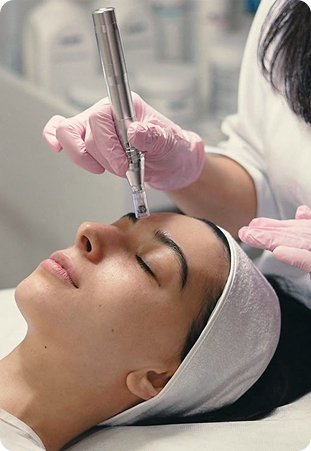
What video does well: visible skin conditions (rashes, acne, eczema, suspected shingles, wound healing), eye redness and discharge, lip and mouth lesions, posture and gait, breathing rate and effort, swelling, the appearance of injuries, and your general clinical picture. Doctors are trained to gather a remarkable amount of diagnostic information from a careful history plus a focused visual exam.
What video cannot do: listen to your heart and lungs with a stethoscope, palpate your abdomen, look inside your ears or throat with proper instruments, take blood pressure (unless you have a home cuff), or perform pap smears, joint injections, sutures, or imaging. For these your doctor will either order a lab requisition you can use at any community lab, refer you to imaging, or recommend an in-person visit. Bloodwork can be ordered by requisition during a video visit and completed at a local lab.

How to Prepare So Your Visit Runs Smoothly
A few minutes of preparation makes a noticeable difference, especially for first-time patients.
- Have your provincial health card ready — your doctor will need the number to verify identity and bill where applicable. AHCIP cards apply for Alberta residents.
- Write down your symptoms — when they started, how they have changed, what makes them better or worse, and what you have tried. This is the single most useful thing you can do.
- List your current medications — include prescriptions, over-the-counter products, vitamins, and supplements with doses.
- Photograph skin issues in good light — if you have a rash, mole, or wound to show the doctor, take clear close-up photos with your phone before the call. You can hold them up to the camera or upload them.
- Know your pharmacy — name, location, and ideally the phone number, so any prescription can be sent immediately.
- Pick your spot 10 minutes early — quiet room, good light, charged device, and Wi-Fi or strong cell signal. Run a quick camera check.
- Have a notepad ready — to write down dosing instructions, follow-up steps, and any specialist names mentioned.
Privacy and Security on the Video Call
TelePlusCare video visits run on encrypted platforms that meet Canadian healthcare privacy standards under PIPEDA and provincial legislation including Alberta's Health Information Act. Your call is not recorded for marketing, not shared, and not used to train algorithms. Only the physician on the call has access to your consultation.
A few things you control on your end: take the call from a private space, use headphones if others are around, and avoid public Wi-Fi for sensitive conversations when possible (your home network or mobile data is fine). Your doctor will confirm your identity at the start of the call and will not discuss your health with anyone else without your written consent.
Troubleshooting Common Video Visit Problems
Almost every issue patients run into has a quick fix.
- Doctor cannot see you — check your browser has camera permission. On iPhone, this is in Settings > Safari > Camera. On Android, it appears as a popup the first time you open the link.
- Doctor cannot hear you — same idea, but for the microphone. Also check your phone is not on silent and your headphones are not still connected to a different device.
- Frozen or laggy video — close other apps and browser tabs, move closer to your Wi-Fi router, or switch to mobile data. The doctor can also continue by audio if video keeps dropping.
- Echo or feedback — wear headphones or move further from any other device that joined the call.
- Cannot find the link — check your spam folder and your text messages. The link comes from a TelePlusCare-verified sender.
- Running late — call our line and we can usually adjust your start time within the same window.
When a Video Visit Is Not the Right Choice
Video care covers most non-emergency concerns, but some situations need in-person attention or emergency services.
Call 911 immediately for chest pain or pressure, sudden weakness or numbness on one side, slurred speech or facial drooping (signs of stroke — remember FAST: Face, Arms, Speech, Time), severe difficulty breathing, severe abdominal pain, heavy uncontrolled bleeding, anaphylaxis, or thoughts of harming yourself. For mental health crises, you can also reach 9-8-8 (Suicide Crisis Helpline) any time.
Go in person for procedures (suturing, joint injections, IUD insertion), conditions that need a stethoscope or hands-on exam to confirm (suspected pneumonia in an unwell patient, possible appendicitis, complex abdominal pain), and anything where your doctor recommends it after the video assessment. A video visit can still be a useful first step — your physician will tell you exactly where to go next.
Your Fast and Convenient Healthcare Solution
Connect with a licensed healthcare provider from the comfort of your home. No referral needed — book your virtual appointment today.
Book Your Appointment NowServing Communities Across Alberta
Available across Canada — Alberta (AHCIP-eligible), Ontario, British Columbia, Saskatchewan via virtual consultation.
Teleplus care clinic is not an urgent care clinic. If you have an emergency please call 911 or go to the nearest urgent care facility.