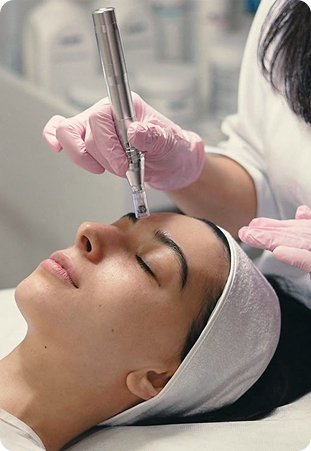
Menopause Treatment in Edmonton — Online HRT Care for Alberta
Hot flashes, night sweats, sleep loss, mood shifts, brain fog, and vaginal dryness — perimenopause and menopause can disrupt almost every part of your day, and Edmonton women often wait many months for a gynecology referral through Alberta Health Services. TelePlus Care offers same-week virtual menopause consultations for women across Edmonton and the Capital Region with licensed Alberta physicians who follow Society of Obstetricians and Gynaecologists of Canada (SOGC) and Canadian Menopause Society (CAMS) guidance. We carefully review your symptoms and personal history, order hormone, thyroid, and metabolic labs through DynaLIFE collection sites, and discuss appropriate hormone therapy options, vaginal estrogen for GSM, and non-hormonal alternatives. Consultations may be covered by Alberta Health Care for AHCIP-eligible residents; medications are not covered.
Book Your Appointment Now
TelePlus Care provides same-week virtual menopause consultations in Edmonton with licensed Alberta physicians following SOGC and CAMS guidelines. We assess perimenopause and menopause symptoms, order hormone, thyroid, and metabolic labs through DynaLIFE, and discuss hormone replacement therapy, vaginal estrogen, and non-hormonal options. Consultations may be AHCIP-covered for eligible Alberta residents.
- Average age of natural menopause in Canada is 51, with perimenopause typically lasting 4 to 8 years before the final menstrual period.
- Hormone therapy options reviewed include systemic estrogen, combined estrogen-progestin (for women with a uterus), transdermal patches, and low-dose vaginal estrogen for genitourinary syndrome of menopause (GSM).
- Care follows the Canadian Menopause Society (CAMS) and Society of Obstetricians and Gynaecologists of Canada (SOGC) 2021 menopause and osteoporosis guidelines.
- Non-hormonal options for vasomotor symptoms include SSRIs/SNRIs (such as venlafaxine or paroxetine) and gabapentin, useful when hormone therapy is contraindicated.
What Is Menopause? Symptoms Edmonton Women Should Know
Menopause is the point 12 months after your final menstrual period — most Canadian women reach it around age 51. The years leading up to it (perimenopause) typically last 4 to 8 years and are when most symptoms begin: irregular cycles, hot flashes, night sweats, sleep disturbance, mood changes, anxiety, palpitations, joint aches, brain fog, and vaginal dryness or painful intercourse (genitourinary syndrome of menopause, GSM).
Surgical menopause (after bilateral oophorectomy), chemotherapy-induced menopause, and primary ovarian insufficiency before age 40 are managed differently and often require earlier hormone therapy. Our Edmonton virtual clinic supports all of these scenarios.
- Vasomotor symptoms — hot flashes and night sweats affect roughly 75 percent of women in the menopause transition.
- Sleep & mood — fragmented sleep, new-onset anxiety, low mood, and irritability are recognized menopause-related symptoms.
- Genitourinary symptoms — vaginal dryness, burning, painful sex, and recurrent UTIs often respond well to local vaginal estrogen.
- Bone & cardiometabolic — estrogen loss accelerates bone density decline and shifts cardiovascular risk; screening matters.

Diagnosis: How We Confirm Menopause Online in Edmonton
For women over 45 with classic symptoms, menopause is a clinical diagnosis — routine FSH testing is not always required, per SOGC guidance. For women under 45, those with atypical symptoms, or those with a history of hysterectomy, we order targeted lab work through Edmonton-area collection sites.
- Hormone panel where indicated — FSH, estradiol, TSH (to rule out thyroid disease, which mimics menopause), and prolactin if cycles are irregular.
- Cardiometabolic baseline — fasting glucose or HbA1c, lipid panel, vitamin D, and ferritin.
- Imaging coordination — pelvic ultrasound at DynaLIFE Medical Labs, Insight Medical Imaging, or Mayfair Diagnostics if abnormal bleeding is reported.
- Bone density (DEXA) — referred for women with risk factors per Osteoporosis Canada criteria.
Treatment Options — Hormone Therapy and Beyond
Treatment is individualized. Hormone therapy (HT) remains the most effective treatment for moderate-to-severe vasomotor symptoms and GSM in appropriate candidates. The Canadian SOGC and Canadian Menopause Society support HT initiation in healthy women under 60 or within 10 years of menopause onset, where benefits typically outweigh risks.
- Systemic estrogen (oral or transdermal) — transdermal patches/gels are often preferred because they avoid first-pass liver metabolism and carry a lower venous thromboembolism (VTE) risk than oral estrogen.
- Combined estrogen + progestin — required for women with an intact uterus to protect the endometrium; micronized progesterone is commonly used.
- Vaginal estrogen — low-dose creams, tablets, or rings for GSM; minimal systemic absorption and considered safe for many women who cannot use systemic HT.
- Non-hormonal — SSRIs/SNRIs (paroxetine, venlafaxine, escitalopram) and gabapentin for hot flashes; ospemifene or DHEA for GSM in select cases.
- Lifestyle — layered clothing, sleep hygiene, weight-bearing exercise, calcium and vitamin D, smoking cessation, and limiting alcohol and caffeine triggers.
Edmonton-Specific Care Pathways
Edmonton women have access to excellent menopause-related diagnostic and specialist resources, but family physician and gynecology wait times can stretch 6 to 12 months in the AHS Edmonton Zone. TelePlus Care helps you start care faster while coordinating in-person services where needed.
- Lab and imaging — DynaLIFE Medical Labs collection sites across Edmonton, Insight Medical Imaging, and Mayfair Diagnostics for ultrasound and DEXA.
- Specialist referrals — University of Alberta Hospital Women's Health, Lois Hole Hospital for Women, and AHS Edmonton Zone gynecology when complex care is required.
- Pharmacies — prescriptions sent to your preferred Edmonton, Sherwood Park, St. Albert, Leduc, Spruce Grove, Beaumont, or Fort Saskatchewan pharmacy.
- Capital Region coverage — virtual visits available across the Edmonton metropolitan area.
The Virtual Menopause Consultation Process
Your first visit usually runs 20 to 30 minutes and is followed by a structured care plan. Follow-up is scheduled at 6 to 12 weeks to assess response and adjust dosing.
- Step 1 — Book online at telepluscare.com or call 587-442-4898; complete a structured menopause symptom and medical history questionnaire.
- Step 2 — Secure video or phone consult with a licensed Alberta physician to review symptoms, contraindications, and goals.
- Step 3 — Lab requisition issued (where indicated) for FSH, TSH, lipid panel, fasting glucose, and other relevant tests at a DynaLIFE site.
- Step 4 — Personalized treatment plan: hormone therapy, non-hormonal options, lifestyle counselling, and a written care plan; follow-up at 6 to 12 weeks.

When You Need a Specialist Referral
Most uncomplicated menopause care can be safely managed virtually by a family physician. We refer to specialists when the clinical picture warrants it.
- Gynecology — abnormal uterine bleeding, persistent postmenopausal bleeding, suspected fibroids or polyps, or HT failure after appropriate trial.
- Endocrinology — premature ovarian insufficiency, complex thyroid disease, suspected adrenal disorder, or unusual lab patterns.
- Breast health — referral for diagnostic mammogram and surgical consultation if a breast lump or imaging abnormality is found.
- Cardiology — for women with established cardiovascular disease before initiating systemic estrogen.
Cost & Coverage in Alberta
For AHCIP-eligible Alberta residents, the medical consultation may be covered by Alberta Health Care. The medications themselves — including hormone therapy patches, oral estrogen, progesterone, vaginal estrogen, SSRIs, and gabapentin — are NOT covered by AHCIP. Many products are partially or fully covered by employer drug plans, Alberta Blue Cross, or Non-Group Coverage. Out-of-pocket costs vary widely; transdermal estradiol patches and micronized progesterone are typically the most expensive components.
Why Choose TelePlus Care vs. Waiting for AHS Gynecology
AHS Edmonton Zone gynecology referrals frequently take 6 to 12 months. Symptoms shouldn't have to wait that long. TelePlus Care offers same-week virtual visits with licensed Alberta family physicians experienced in menopause management, and we escalate to gynecology when truly needed.
- Same-week virtual appointments across Edmonton and the Capital Region.
- SOGC and CAMS guideline-based care from licensed Alberta physicians.
- Lab and imaging coordination through DynaLIFE, Insight Medical, and Mayfair Diagnostics.
- Honest, evidence-based discussion of HT benefits, risks, and contraindications including breast cancer history and VTE risk.
Your Fast and Convenient Healthcare Solution
Connect with a licensed healthcare provider from the comfort of your home. No referral needed — book your virtual appointment today.
Book Your Appointment NowServing Communities Across Alberta
Edmonton, Sherwood Park, St. Albert, Leduc, Spruce Grove, Fort Saskatchewan, Beaumont, and surrounding Capital Region.
Teleplus care clinic is not an urgent care clinic. If you have an emergency please call 911 or go to the nearest urgent care facility.