Eczema Treatment Online in Canada — Virtual Prescriptions
Eczema treatment online with TelePlus Care helps Canadians stop the itch-scratch cycle without waiting weeks for a clinic visit. Our licensed physicians assess flares through secure video and photo upload, identify likely triggers — from winter dryness to detergents and fragrances — and build a stepped plan that combines a daily emollient routine with prescription anti-inflammatory medication when needed. Treatments may include hydrocortisone, betamethasone, tacrolimus, pimecrolimus, or oral antihistamines for sleep-disrupting itch. We issue a prescription you can fill at any pharmacy in Canada, and most patients see a meaningful reduction in redness, itching, and weeping within two weeks.
Book Your Appointment Now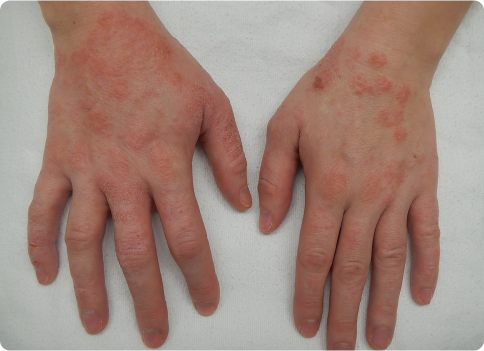
Eczema treatment online connects Canadians with licensed physicians who diagnose atopic dermatitis through secure video and photo review. Doctors can issue prescriptions for topical corticosteroids, calcineurin inhibitors, barrier-repair moisturizers, and oral antihistamines, which patients fill at any pharmacy. Virtual care speeds access to flare relief without long referral wait times.
- Atopic dermatitis affects roughly 17% of Canadians at some point in their lives.
- Common triggers include cold dry air, harsh soaps, fragrances, dust mites, and stress.
- Treatments include topical steroids, calcineurin inhibitors, emollients, and oral antihistamines.
- Physicians commonly prescribe hydrocortisone, betamethasone, tacrolimus, and pimecrolimus.
What Is Eczema?
Eczema, also called atopic dermatitis, is a chronic inflammatory skin condition marked by dry, itchy, red, and sometimes oozing or thickened patches. It usually starts in childhood, but adult-onset cases are common. The condition stems from a combination of a weakened skin barrier (often linked to filaggrin gene variants), an overactive immune response, and environmental triggers. Canadian winters — with their cold outdoor air and dry indoor heating — are particularly hard on eczema-prone skin. Eczema runs in families alongside asthma and hay fever, the so-called atopic triad. While there is no permanent cure, modern treatments make most cases very manageable.

Symptoms and Where Eczema Appears
Eczema looks different at different ages. Infants often present with red, weeping cheeks and scalp involvement. In children, the inside of the elbows and back of the knees are classic spots. Adults more commonly see hand eczema, eyelid involvement, and patches on the neck and torso. Across all ages, the hallmarks are intense itching, dryness, redness, and skin that becomes thickened (lichenified) where it has been scratched repeatedly. Severe flares can ooze, crust, and sleep can suffer. Our physicians map your distribution and severity to choose the right potency of treatment for each body site.
- Infants: cheeks, scalp, weeping patches
- Children: insides of elbows and behind knees
- Adults: hands, eyelids, neck, torso
- All ages: itch, dryness, redness, thickened skin
Causes and Triggers
Genetics set the stage by weakening the skin barrier, but daily life decides when flares happen. Common Canadian triggers include cold dry winter air, prolonged hot showers, fragranced soaps and laundry detergent, wool fabrics, dust mites, pet dander, and stress. Food allergies are a less common trigger than people assume — they mostly play a role in young children. Our physicians help you identify your personal trigger pattern so you can prevent flares as well as treat them. Simple changes such as switching to lukewarm showers, fragrance-free cleansers, and a thick emollient applied within three minutes of bathing can dramatically improve outcomes.
When to See a Doctor
Book a virtual visit if eczema is interfering with sleep, spreading, oozing or crusting, not responding to OTC moisturizers and 1% hydrocortisone after two weeks, or recurring frequently. Sudden painful blistering, fever, or yellow crusting can signal infection (bacterial or eczema herpeticum) and needs prompt attention. Our physicians will tell you whether a virtual visit is appropriate or whether you need to be seen in person — and we will refer you for an in-person dermatology assessment if your case is severe, atypical, or you may benefit from advanced therapies such as biologics or phototherapy.

Treatment Options
Eczema treatment is layered. Daily emollients are the foundation — thick creams or ointments applied generously, twice a day, lock in moisture and repair the skin barrier. For active flares, topical corticosteroids (hydrocortisone for the face and folds; betamethasone or mometasone for the body) calm inflammation quickly. Topical calcineurin inhibitors like tacrolimus and pimecrolimus are steroid-free options that work well on the eyelids and other delicate areas. Oral antihistamines can help with sleep when itch is severe. Severe or stubborn cases may benefit from phototherapy or systemic therapies such as dupilumab, which require in-person dermatology referral.
- Daily: fragrance-free emollients applied generously
- Flares: topical steroids matched to site and severity
- Sensitive areas: tacrolimus or pimecrolimus
- Severe: phototherapy or biologics via referral
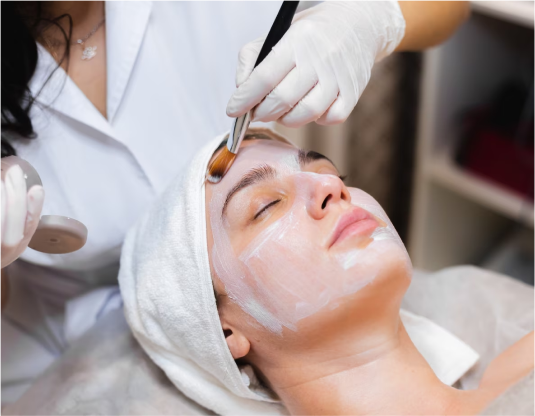
How a Virtual Eczema Consultation Works
Choose a slot, complete a brief health questionnaire, and upload photos of the affected areas in natural light. On the video call, your physician examines the patches, asks about flare patterns, current skincare, and triggers, and rules out look-alikes such as contact dermatitis or psoriasis. If a prescription is appropriate, the doctor issues a prescription you can fill at any pharmacy. We recommend follow-up at 2-4 weeks to confirm the flare is settling and to step down treatment safely. The consultation may be covered by AHCIP for Alberta residents; specialty creams and prescription medications are not covered.

What to Expect From Your Prescription
Topical steroids usually reduce redness and itch within 3-7 days. Use them only on active patches and follow the duration your physician sets — typically 1-2 weeks for stronger steroids on the body, shorter for the face. Tacrolimus and pimecrolimus may sting for the first few applications and then settle; effects build over 1-2 weeks. Continue your emollient even after the flare clears — daily moisturizing prevents the next flare. Tell your physician right away if the rash worsens, develops yellow crust, or spreads, since infected eczema needs different treatment.
Your Fast and Convenient Healthcare Solution
Connect with a licensed healthcare provider from the comfort of your home. No referral needed — book your virtual appointment today.
Book Your Appointment NowServing Communities Across Alberta
Canada-wide for Ontario, British Columbia, Saskatchewan; consultation services in Alberta.
Teleplus care clinic is not an urgent care clinic. If you have an emergency please call 911 or go to the nearest urgent care facility.